Investors are making a fortune from UK healthcare. Why is nobody holding private equity to account?
From care homes to cancer treatment, millions are being siphoned out of the system every year – usually to the detriment of services
How private finance is crippling health and social care
Private Finance Initiative (PFI) costs continue to grow in the NHS, even as other healthcare budgets are stretched further and profits extracted.
Capital spendingcare homesPFIPrivate equityPrivate Finance Initiative
Paying for Healthcare on the “Never, Never” in the UK – how has it come to this?
At the heart of the social contract underpinning the NHS is that healthcare in the UK should be provided on the basis of need rather than ability to pay.
The crisis in general practice: Continuity of care vs ‘transactional’ care
This post is the third of a three-part on the state of primary care, focusing on the type of care GP’s provide.
The Crisis in Primary Care: The GP Shortage
The second of a three part series on the State of Primary Care
The Future of Primary Care: Threats and Opportunities
The first of a three part blog series on the state of primary care by two of CHPI’s founding Trustees.
Is treating private patients a net benefit to NHS Trusts? We may never know
In April 2022 draft NHS England planning guidance told NHS Trusts that ‘private patient services continue to be a significant source of material opportunity for the NHS.’ But CHPI research from 2018 has shown that this is not necessarily the case.
PPUsPrivate Healthcareprivate hospitalsPrivate Patient UnitsRoyal Marsden
Reflecting on medical scandals and their impact on women
Discussing CHPI’s recent screening of ITV’s “Bodies of Evidence” – an uncomfortable documentary covering the activities of the convicted breast surgeon Ian Paterson.
AccountabilityIan PatersonPatient safetyPatient safety in private hospitalsRegulationWhistleblowing
Thousands of women have been harmed as a result of patient safety scandals, particularly in the private sector – what explains the lack of action by Government?
In this blog, David Rowland discusses the ongoing scandal of patient safety in private hospitals, and why so many women in particular have been affected by negligent medical practice and regulation.
Ian PatersonPatient safetyPatient safety in private hospitalsprivate hospitals
Smoke and Mirrors: NHS England’s ‘totally transparent’ multi-billion pound deal with the private hospital industry
Despite promises to the contrary, NHS England still hasn’t even attempted to be transparent about its last round of contracts with the private sector.
“Living with the virus”—let’s not forget government accountability amid narratives of personal responsibility
Positioning the next stage of the pandemic as a matter of “learning to live with” covid-19 suits those who do not want to be held accountable for what has happened
Private hospitals have no doctors
The idea that the private sector is helping the NHS to deal with the aftermath of the COVID pandemic is a myth.
Conflicts of interest in the post Lansley NHS—from a regulated to an unregulated healthcare market?
David Rowland questions the common perception that the latest Government’s proposals for NHS reform represent a turn away from private sector involvement in the NHS and the market-based orthodoxy in health policy.
Farewell to the NHS market
Professor Calum Paton argues the integration outlined in the government’s NHS white paper is not as “innovative” as its title might suggest
At this time of crisis, profiting from scarce NHS resources is unconscionable
If there is any hope of providing a comprehensive hospital service right now, every hospital bed and every consultant should be placed under the direct control of the NHS and care should only be available on the basis of need not ability to pay.
International trade and the public interest
Are public interests at risk from the trade and investment agreements (TIAs) the UK is currently negotiating to replace its previous deals as a member of the EU? In particular, what about the public interest in the NHS as a publicly provided, publicly accountable, universal service, free at the point of delivery?
There is an urgent need to review the UK’s system of communicable disease control administration and its public health laws
In the midst of a lethal pandemic, the government controversially axed the main public health body (Public Health England) and announced the creation of yet another bureaucracy, designed by management consultants with no expertise in public health. History shows that without a clear overarching strategy and laws, these ad hoc reforms are likely to further hamper the UK’s ability to protect the population.
Undermining public law is no way to protect public health
David sets out worries about how coronavirus is being used to suspend or ignore safeguards designed to protect the public interest. Originally posted in OpenDemocracy
Some financial conflicts of interest in medicine cannot be managed and should be prohibited
David considers the recommendations of the Cumberlege review in BMJ Opinion
COVID-19 and BAME inequalities – the problem of institutional racism
Do Public Health England’s BAME reviews fail to directly address racism as a driver of health inequality?
Healthcare staff struggled to speak out long before COVID-19. They need help to do so now
While healthcare workers fight on behalf of us all against COVID-19, they can still risk their jobs for blowing the whistle on dangerous practices and wrongdoing.
After PPE and testing, contact tracing looks like the next government shambles
In his latest piece for the Guardian, CHPI’s David McCoy exposes the failings of the UK’s contact tracing efforts
The hidden profits behind collapsing care homes
The opaque financial structure of the major care home groups means that they are more vulnerable to collapse and enable hidden profits to leak out.
Coronavirus has exposed the dangerous failings of NHS marketisation
CHPI Trustee David McCoy writes for the Guardian about how the 2012 Lansley Act underlies some of the failings in the UK’s response to COVID-19.
To protect older people from COVID-19, state coordination of the social care sector is urgently needed
CHPI Director David Rowland writes for LSE Policy & Politics about the urgency of a more co-ordinated response in the highly fragmented social care sector.
What can the UK learn from South Korea’s response to COVID-19?
Senior Lecturer in Global Public Health Jonathan Kennedy considers South Korea’s extensive use of testing and tracing in place of large-scale confinement or travel restrictions.
What exactly is the government strategy for COVID-19, and is it right?
Prof David McCoy considers the UK government’s approach to controlling the disease, the health system, and the social and economic impacts.
Who benefits from the NHS’s bailout of private hospitals?
The government’s recent deal with private hospitals, who will provide their beds and staff to help the NHS cope with coronavirus, has been framed as a significant boost for the NHS. But the larger benefits are arguably for the private hospitals themselves and their lenders and landlords, who in effect have received a bailout from the government at a time of crisis.
Behind the Curve – how a focus on cost reduction and competition has left the NHS unable to protect the population’s health
Policy makers have known about the likelihood and impact of a virus like COVID-19 for many years. And yet the risks to population health have barely received a mention in long-term planning for the NHS over the last decade.
The Paterson inquiry is a missed opportunity to tackle systemic patient safety risks in private healthcare
In this piece, published today in BMJ Opinion, CHPI Director David Rowland sets out how he sees the Paterson Inquiry’s report as yet another missed opportunity to tackle the systemic patient safety risks which lie at the heart of the private hospital business model.
What should be in the election manifestos on health and social care?
In the run up to the December 2019 election ─ held at a time when the NHS and social care are typically under strain ─ CHPI Director David Rowland outlines a number of key policies that the party manifestos should include if the various crises in the sector are to be addressed by the next government.
AccountabilityMarketisationNHS & Social Care FundingWorkforce
Flawed data? Why NHS spending on the independent sector may actually be much more than 7%
In this piece for LSE Politics & Policy, David explains how flaws in the presentation of data on NHS expenditure prevent policymakers from having a clear understanding of where money within the system is going.
Unconstitutional governance of the NHS in England – a symptom of the UK’s political malaise
As the political crisis tips over into a full blown constitutional crisis, the NHS in England remains highly susceptible to the ditching of constitutional conventions.
Mary Greaves – ‘My brother Peter’
Mary Greaves, the sister of Peter O’Donnell, gave this moving account of Peter’s death following treatment as an NHS patient in a private hospital to an audience at the HSJ Patient Safety Congress in Manchester in July 2019.
"Life in the front line" seriesPatient safetyPatient safety in private hospitals
The NHS’s workforce shortages illustrate the UK’s dependence on migrant labour
The NHS’s persistent dependence on migrant labour is a reflection of the structure of the wider UK economy.
Addressing the funding gap for NHS trauma care – ensuring that the insurance industry pays its fair share
Are insurers paying their fair share for trauma care provided by the NHS? This blog calls for a review to ensure that the NHS is being fully compensated.
The case of Circle vs. the NHS – why NHS and private providers do not compete on a level playing field
Circle’s lawsuit against an NHS CCG illustrates the flaws in financially comparing private and NHS providers.
Corporate care home collapse and ‘light touch’ regulation: a repeating cycle of failure
In light of the care home chain Four Seasons going into administration , CHPI Director David Rowland looks at the failure of the regime designed to prevent such situations, as well as the cause of the collapse.
Brexit and the NHS – the risk to the provision of healthcare as a fundamental matter of human dignity
The toxic debate about Brexit has inevitably spilled over into discussion about the future of the NHS. But have we fully quantified the risks to the NHS’s founding principles?
Is this the way the future’s meant to feel? The NHS Long Term Plan and the future of health and social care in England
CHPI’s new Director offers a cutting critique of Simon Stevens’ new NHS Long Term Plan
Patients as co-producers of heath
In our third of three essays in honour of Julian Tudor Hart, Jonathan Tomlinson considers his passionate advocacy for partnerships with patients, shared understanding and shared decision making, long before it was the subject of editorials in the British Medical Journal and international conferences.
Too much trouble, or bad for business? The private sector’s attitude to an effort to improve patient safety
A commentary on the findings of an enquiry by the Royal College of Anaesthetists into how well prepared hospitals are to deal with perioperative anaphylaxis shock
Primary care and technological innovation
Jens Foell considers how Julian Tudor Hart’s work bears on the relationships between medicine, social justice and technology
Essays in honour of Julian Tudor HartTechnological innovation
The Private Health Information Network (PHIN): a missed opportunity
Dual qualified medical doctor and solicitor Jock Mackenzie explains the severe failings he sees in the PHIN’s work to provide patient safety data for private hospitals
Julian Tudor Hart and the essence of primary care
The first of three essays in honour of Welsh GP Julian Tudor Hart – whose research and practice have lots to teach us about contemporary primary care challenges
Reflections on medical culture and the Bawa Garba case
Jonathon Tomlinson reflects on the systematic and cultural problems around managing errors and mistakes in healthcare highlighted by the case of Dr Bawa-Garba
Just wanting a “just culture”
Dr Jenny Vaughan reflects on the case of Dr Hadiza Bawa-Garba and charges of gross negligence manslaughter in medical cases.
The NHS must stop excluding immigrant patients while poaching health workers from abroad
Seventy years ago this month the NHS was founded with the promise that its care would be free at the point of delivery, and patients would be treated solely on the basis of need. Over the last few decades, both principles have been progressively violated.
Comparing the NHS with other health systems: things to keep in mind
As the NHS turns 70 there is great interest in comparisons between the NHS and other health systems, but what key points need to be kept in mind?
AccountabilityMarketisationPerformance EvaluationService reconfiguration
Whistleblowing in the NHS isn’t fixed yet, and this leaves patients exposed
In the wake of the Gosport War Memorial Hospital case, Dr. Minh Alexander considers how free NHS workers really are to speak up when they have concerns about patient safety.
Risks to the NHS when referring to private hospitals
The time has come for the NHS corporately, and referring clinicians individually, to consider their own responsibility for the safety of NHS patients in private settings.
Are GPs referring too many patients? If so, why?
Jonathan Tomlinson considers the competing pressures faced by GPs in their role as gatekeepers to other NHS services.
The Ian Paterson case and the Fraud Act 2006: a potential case of corporate liability?
It is arguable that Spire Parkway and/or its employees could be held criminally accountable for an offence under section 2 of the Fraud Act 2006.
Can regulation prevent another Ian Paterson or is more radical reform needed?
Our take on the latest CQC report on Independent Acute Hospitals.
AccountabilityPatient safetyPatient safety in private hospitals
Treating private patients in NHS hospitals – benefit or cost?
An independent investigation is needed into whether trusts are getting significant net additions to their income from treating private patients, and whether the drive to set aside yet further beds for private patients should be allowed to continue.
London’s hospital and school PFI schemes
With interest in a greater role for City Hall in London’s NHS this data blog looks at the extent of PFI payments in the city.
Counting the cost of school PFI schemes
This blog extends CHPI’s existing analysis on PFI in the NHS to look at the education sector in England, and potential avenues for saving taxpayers’ money.
Fake news about the NHS
Misuse of information in discussions about the spending and performance of the NHS is all too common: the future of the NHS relies on getting the basic facts right.
AccountabilityInformationNHS & Social Care FundingPerformance Evaluation
Lives at risk: The government’s inadequate management of coroners’ warnings about the NHS
To avoid unnecessary future deaths we must ensure that coroners’ warnings about the NHS are heeded
With PFI our hands are tied – so what can be done?
Taken together, the collapse of Carillion and the National Audit Office’s report on the legacy of PFI and PF2 should be the final nails in the coffin of the use of private finance to fund public infrastructure projects. But what can we do about existing contracts?
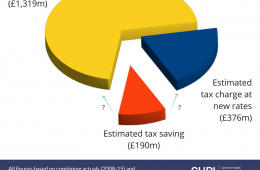
The PFI companies’ windfall from falling Corporation Tax rates
What is the basis for imposing a windfall tax on PFI operating companies and what sum could be reasonably expected?
The light inside has broken but I still work
Crisis in the NHS means patient safety and the well-being of the work force are at stake. Medical leaders and politicians must take responsibility.
"Life in the front line" seriesFront line careNHS & Social Care FundingNHS Crisis
NHS hospital subsidies to private hospitals
How widespread is the practice of NHS hospitals providing clinical cover to private providers, and what reimbursement does the NHS receive for providing these services?
Ian Paterson and the confiscation of the proceeds of crime
Could the Proceeds of Crime Act 2002 be used to recuperate money from the disgraced breast surgeon Ian Paterson and his employer, Spire Healthcare?
‘Footprints’ that leave no footprints: unaccountable policy-making for the NHS in England
Difficulties in obtaining complete and reliable data from STP teams regarding transition planning reflect the inherently unaccountable nature of the STPs themselves.
Do we need to invest more in NHS administration?
Vivek Kotecha argues that there needs to be greater investment in administration to ensure a well-run NHS for both patients and staff.
Implications of the Ian Paterson case for the private hospital sector
After the breast surgeon was sentenced to 15 years for performing unnecessary operations on cancer patients, Colin Leys considers what the inevitable inquiry could mean for private hospitals.
AccountabilityPatient safetyPatient safety in private hospitals
Speaking up for a public NHS
There are 60 million “key stakeholders” in our NHS in the UK who need to be listened to: As an NHS junior doctor and patient, I – alongside many others – can no longer tolerate being excluded from the vital public conversation about the future of the NHS.
Our NHS has a staff shortage — and Brexit could make it worse
In the context of Brexit, attention must be paid to what a cap on migration means for recruiting and retaining the NHS workforce.
Why the Dilnot cap is not the answer to the social care funding crisis
Social care requires a significant injection of public funds to move from being a residual public service to one which enhances the lives of older people. Until then, the crisis will continue to worsen.
The impact of poverty on the health of our children
A new report suggests that by 2020 5 million children in the UK will be living in poverty. Paediatrician Guddi Singh explains the devastating impact this will have on these children’s health and calls on the Government to act.
What do Sustainability and Transformation Plans mean for continuity of care within the English NHS?
Few STP proposals recognise the complexity of continuity of care. We must demand that STPs recognise the necessary thought and resources required to implement new regimes of continuity of care effectively.
The past, present and future health costs of inequality
We must act on evidence that shows childhood trauma risks the development of disease in later life.
STPs – An Opportunity for Much Needed Health System Transformation
A balanced assessment is required if the opportunities presented by the Sustainability and Transformation Plans are to be seized upon.
Will limiting the costs in clinical negligence claims make patients less safe?
The DH’s objective is to reduce the cost of clinical negligence cases so that savings can be invested in patient care. But these proposals risk human and financial costs.
How trustworthy is NHS Digital?
How an argument between the chair of HSCIC (now NHS Digital) and the Home Office / DoH called into question the HSCIC’s trustworthiness as guardian of the personal details of every NHS patient in England.
Why did so many more older people die in England and Wales in 2015?
For almost all of the post-war period, death rates have been falling steadily in England and Wales. Yet 2015 saw the third largest year-on-year rise, with no immediate explanation.
STP Teams – Problems of Legal Status and Accountability
The idea that more competition would improve the NHS is history. But what are the challenges for an approach based on partnership and collaboration?
Life in the front line: a junior doctor’s view
A senior trainee anaesthetist’s perspective on a survey of the welfare and morale of trainee doctors.
Examining the Work, Health and Disability Green Paper
The government’s Green Paper on work, health and disability proposes a plan for helping disabled people into employment, an ambition that initially appeared in the Conservative Party manifesto in 2015.
Santa’s Transformation Plan (STP)
The past 20 years have been trying ones for Santa Claus and the National Elf Service. The decision to split the purchasing of presents from their delivery was meant to improve efficiency, but he’s been having second thoughts…
Defending public health against ‘nanny state’ accusations: we need to talk about freedom
‘Nanny state’ accusations can function as powerful rhetorical weapons against interventions that are intended to benefit people. This blog, based on our recent academic paper, offers suggestions both to help public health advocates develop effective defences against nanny-state accusations and to ensure that public health interventions are well justified.
The future of the QOF in primary care: Lessons from the diabetes story
The Quality and Outcomes Framework (QOF), the pay-for-performance protocol in general practice, has been the subject of significant debate since it was rolled out in 2004. At the core of the debate is whether the quality of general practice can be quantified for the purposes of performance management.
Will boosting the number of ‘home-grown’ doctors make us self-sufficient?
Vivek Kotecha examines whether the government’s announcement of 1,500 extra medical school places will make the UK self-sufficient in doctors given the staffing issues faced by the NHS.
Brexit: the NHS after the referendum
The vote to leave the EU has created a context of profound political and economic uncertainty. What does this change of circumstances mean for the future of the NHS?
Personalisation in healthcare and adult social care: between marketisation and social justice
In this analysis, we set sensationalist headlines about the use of personal budgets aside and concentrate on the tension between two distinct aspects of personalisation – its claims to promote social justice and its commitment to marketisation.
Quality in general practice: measuring vs. improving
Jonathon Tomlinson reflects on the difficulties of measuring the quality of general practice and the prospects of improvement.
The new system of Medical Examiners and the certification of deaths: how much of an advance?
Robert Dingwall looks at the implications for families and for international comparisons of mortality statistics.
Adapting primary care to the GP crisis
Jonathon Tomlinson on the GP crisis and 7-day working.
Celebrity philanthropy and the subversion of the public interest
John Mohan about the need for caution and regulation when public policy comes face to face with philanthropy.
The Medical Innovation Bill: Could this be the most bizarre health Act ever?
Peter Walsh on the dangers of the Medical Innovation Bill.
The social construction of mortality data
Are the relatively high English death rates from cancer a statistical illusion?
Insurance against Clinical Negligence for Private Providers of NHS Care
A private company’s negligence can lead to heavy costs for the taxpayer.
Unresolved safety issues in private hospitals
Dr Lorcan Sheppard critiques gaps in accountability
NHS outsourcing – ‘Netcare revisited’
Have lessons been learnt from patient safety lapses amongst private healthcare providers?
ContractingPatient safetyPatient safety in private hospitals
The risk of fraud in the new NHS: lessons from the USA and the need for a response in England
Professor Mark Button and Dr Martin Tunley examine whether there is enough action on fraud.
Reflections on the Barker Commission
Exploring the proposals in the report
The limits of aggregate performance ratings
Will CQC ratings really tell patients how well a service is doing?
What has devolution meant for the NHS in Scotland and England?
On the eve of the Scottish referendum, Matthew Dunnigan asks what devolution has meant for the NHS in both Scotland and England.
Outsource first, evaluate later
Nick Taylor surveys the impact of outsourcing welfare programmes, and Marianna Fotaki considers the lessons for the NHS
ContractingInequalityMarketisationPerformance EvaluationPublic health
Patient safety in private hospitals
Peter Walsh outlines the discrepancies in patient safety requirements for private health providers
Transforming the culture of healthcare: sick doctors and the GMC
Dr Jonathon Tomlinson critiques recent reports on the role of the General Medical Council
The NHS in Wales: a report from the death zone
Welsh GP Dr Julian Tudor Hart examines what healthcare in Wales has achieved in the face of spending cuts
What next for public accountability in the Scottish NHS?
Ellen Stewart appraises public involvement in the Scottish NHS.
The Future of Primary Care
Dr Jonathon Tomlinson outlines what the future GP practice could look like
Precarious work and mental health
Elizabeth Cotton on difficult working conditions for mental health professionals.
Why service reconfiguration cannot be the solution to the ills of the NHS
Roger Steer looks at why NHS reconfiguration will not solve the problems in the NHS.
Patient-Centred Care: Rhetoric and reality
Dr Jonathon Tomlinson looks at what patient-centred care really means.
The business of older people’s mental health
Martin Blanchard on how older people are losing out with more competition in mental health services.
Care.data: doubts about opting-out
Justine Schneider discusses her doubts about the NHS care.data scheme
What would an evidence-based response to Mid-Staffordshire look like?
Ian Greener reflects on mid-Staffordshire a year on.
Our health and their development: overlapping interests?
Sally Ruane reflects on a recent workshop exploring the synergies between tax and health.
Are health inequalities still a policy priority in the UK? Reflecting on post-1997 experiences and imagining some alternative scenarios
Kat Smith looks at whether health inequalities really are still a policy concern.
Taking action on sugar – applying lessons from the salt reduction programme
Dr Malhotra looks at the role of sugar in the obesity epidemic and calls for urgent action to reduce its consumption based on the success of the salt reduction campaign.
The tyranny of preventative medicine
Dr. Jonathan Sleath looks at the problems with preventative medicine from a GP’s perspective.
On compassion, markets and ethics of care
CHPI’s Marianna Fotaki looks at what is missing from the Government’s response to the Francis Report.
The lobbying bill and the influence of commercial health lobbyists
Tamasin Cave finds that the Transparency of Lobbying Bill would do nothing to expose the influence of commercial health lobbyists while stifling democratic campaigning.
Charging at what cost?
CHPI’s Sally Ruane looks at the Government’s proposals to charge non-EU residents for health care.
The looming gap in NHS funding – what is the government’s policy for dealing with it?
Colin Leys looks at the likely ramifications of the NHS funding gap.
Whistleblowers are essential for safe care
Roger Kline writes about the vital role of whistleblowers in the NHS.
“Too big to fail”? Care home closures and the price of market failure
CHPI talks about the shortcomings in the Care Bill’s approach to the risk of market failure
The Care bill, the duty of Candour and fraud in the new NHS Market
CHPI talks about a missed opportunity by the Government to tackle fraud in the Care Bill.
AccountabilityHealthcare fraudMarketisationSocial careSocial care markets
Private companies paying for access to NHS patients: a view from the maternity ward
A trainee midwife talks about the recent debate about the presence of Bounty on NHS maternity wards
A new think tank
Dr Jonathon Tomlinson talks about the important role for the CHPI.